Table of Contents
Overview – ENT Examination
The ENT examination (ear, nose and throat) is a core clinical skill in both general and specialist medical settings. It plays a critical role in evaluating common patient complaints such as hearing loss, facial pain, sinus pressure, sore throat, or suspected infection. This high-yield OSCE station requires a structured approach covering inspection, palpation, otoscopy, hearing tests, and sinus examination. This guide walks through each step and highlights key clinical signs and differentials for final-year medical students.
Introduction
- Wash hands, introduce yourself, and gain informed consent
- Explain the examination and ensure the patient is comfortable and seated upright
General Inspection
- Observe hair distribution:
- Hirsutism (PCOS, hypothyroidism)
- Oily hair (hyperthyroidism, acromegaly)
- Dry hair (hypothyroidism)
- Look for scars or deformities: trauma, cleft lip, prior surgeries
- Assess facial features:
- High-arched palate (Marfan syndrome)
- Abnormal facies (Cushing’s, Addison’s, Graves’, Down’s, Turner’s)
- Assess skin:
- Lesions (basal cell carcinoma, squamous cell carcinoma)
- Pigmentation (Addison’s, haemochromatosis, acanthosis nigricans)
- Scaling (psoriasis, autoimmune)
- Check facial symmetry, muscle fasciculations, and eye signs:
- Pallor (anaemia), icterus, conjunctivitis, discharge, periorbital oedema
Vital Signs
- Pulse: Tachycardia (infection), bradycardia (raised intracranial pressure)
- Blood pressure: Hypertension may suggest increased ICP
- Respiratory rate: Bradypnoea in raised ICP
- Temperature: Fever indicates infection
Ear Examination
Inspection
- Look for redness (infection), swelling (gouty tophi), scars, lesions (BCC/SCC), and discharge
Palpation
- Tug test: pain indicates otitis externa
- Cervical lymphadenopathy → infection or malignancy
Otoscopy
- Pull pinna upward and backward
- Examine left ear with left hand, right ear with right hand
- Observe for:
- Otitis externa (red, swollen canal)
- Tympanic membrane inflammation, bulging (otitis media)
- Normal landmarks: malleus, light reflex, pars flaccida and tensa
- Signs of chronic disease: sclerosis, rupture
- Cerumen impaction


Hearing Tests
- Whisper test: e.g. “69” and “100” while masking other ear
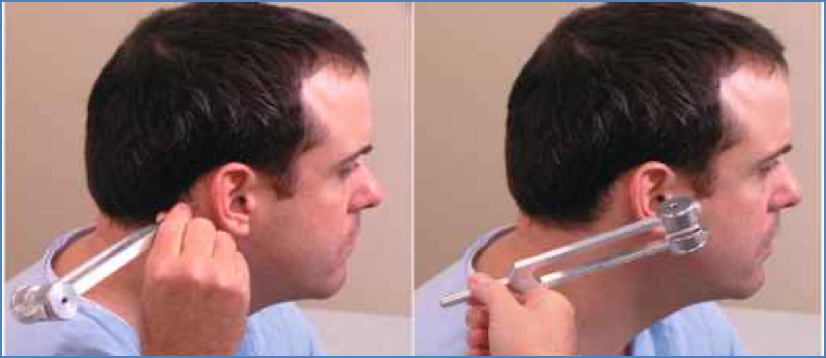
- Weber’s test: Lateralisation suggests conductive (towards affected) or sensorineural (towards normal) loss
- Rinne’s test: Air > Bone (normal); Bone ≥ Air suggests conductive loss



Nose Examination
Visual Inspection
- Look for:
- Redness, acne rosacea, skin cancers (BCC, SCC)
- Scars, deformity, nasal deviation
- Nasal polyps, septal defects
- Discharge (pus, blood), inflamed turbinates
Palpation
- Assess for tenderness or obstruction
- Sinus examination:
- Percuss frontal and maxillary sinuses
- Transilluminate maxillary sinuses (dull = sinusitis)
Throat Examination
Visual Inspection
- Assess:
- Hydration status
- Cyanosis (central or peripheral)
- Oral lesions: ulcers, leukoplakia, petechiae
- Pigmentation (Addison’s), angular stomatitis
- Glossitis, gingival changes (hyperplasia, bleeding – AML, methotrexate)
- Dentition and dead teeth (cardiovascular risk)
- High-arched palate (Marfan’s)
- Tonsillar swelling, exudate, pharyngeal inflammation
- Palatal movement on “Ah” (IX & X nerve integrity)
- Halitosis (uraemia, liver disease, ketosis)
Palpation
- Bimanual exam for parotid swelling
- Palpate tongue and buccal mucosa for lumps
- Examine cervical lymph nodes
Summary – ENT Examination
The ENT examination is a structured assessment vital for evaluating head and neck pathology. It involves inspection, otoscopy, sinus testing, hearing checks, and oral examination — all essential for OSCEs and clinical rotations. For a broader context, see our Clinical Skills Overview page.