Table of Contents
Overview – GI Tract Anatomy
The GI tract anatomy resembles a continuous muscular tube extending from the mouth to the anus. Along its path, the tract includes specialised anatomical regions and histological adaptations tailored to specific functions such as ingestion, digestion, absorption, and defecation. This guide breaks down the key anatomical and microscopic structures from the oral cavity to the rectum, providing a foundational reference for clinical understanding.
Oral Cavity & Pharynx
Key Structures
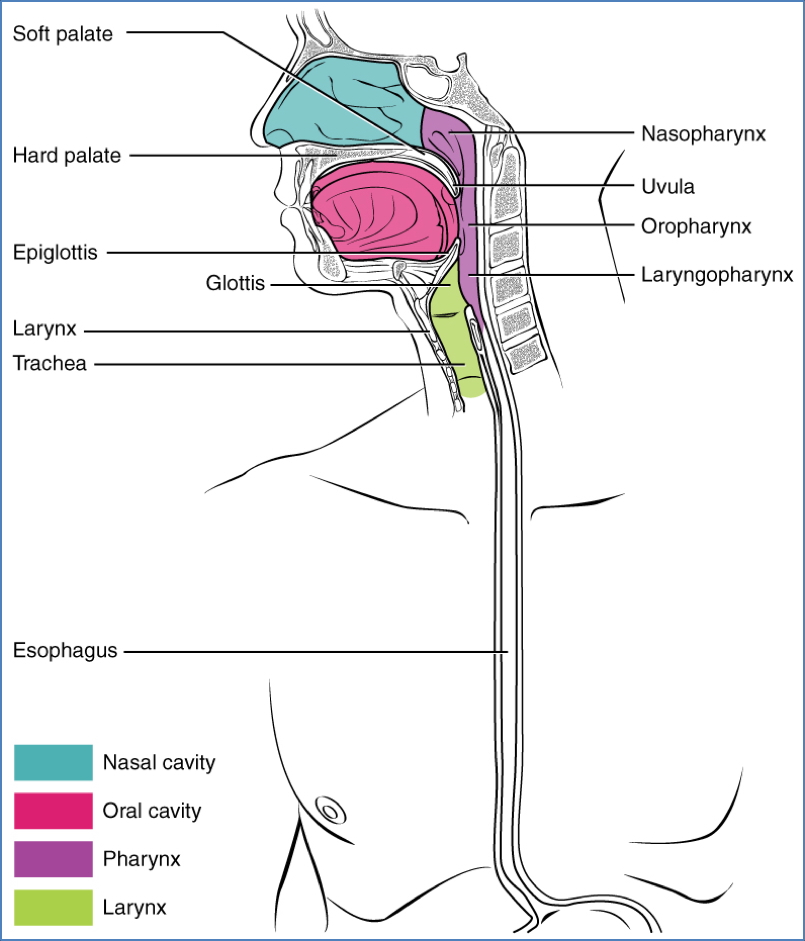
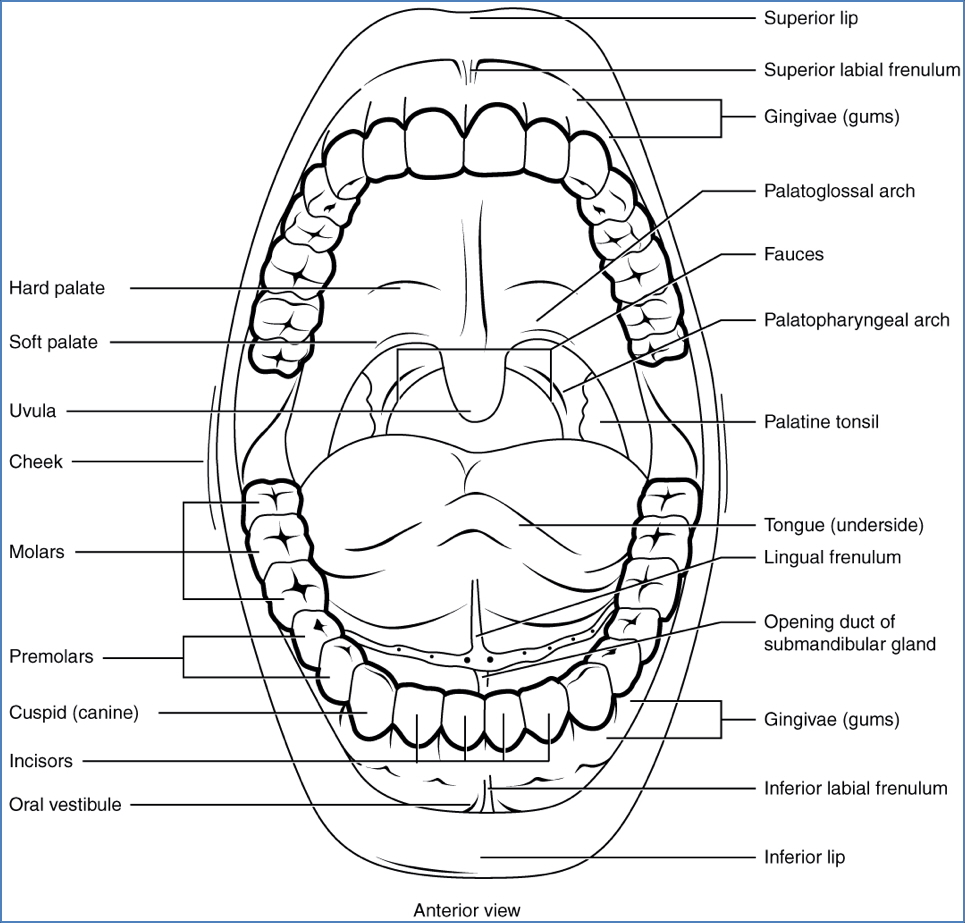
- Lips & Gingiva: Upper/lower lips, labial frenula (lip bridles), gums
- Palate: Hard and soft palate, uvula
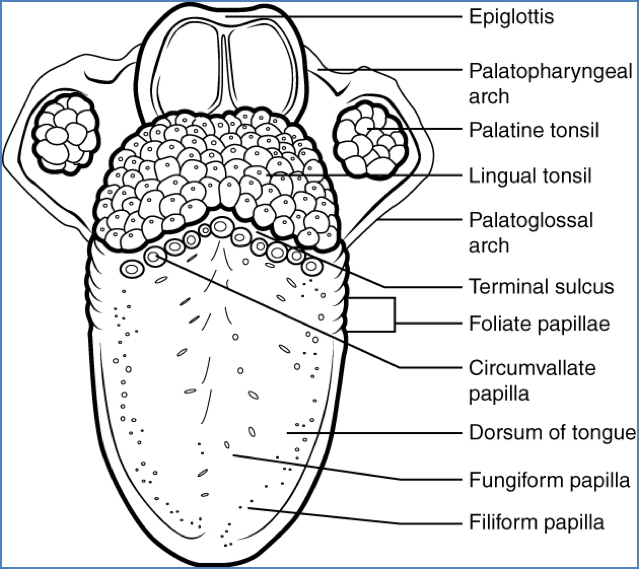
- Tonsils: Pharyngeal, palatine, lingual
- Tongue: Dorsum, root, lingual frenulum
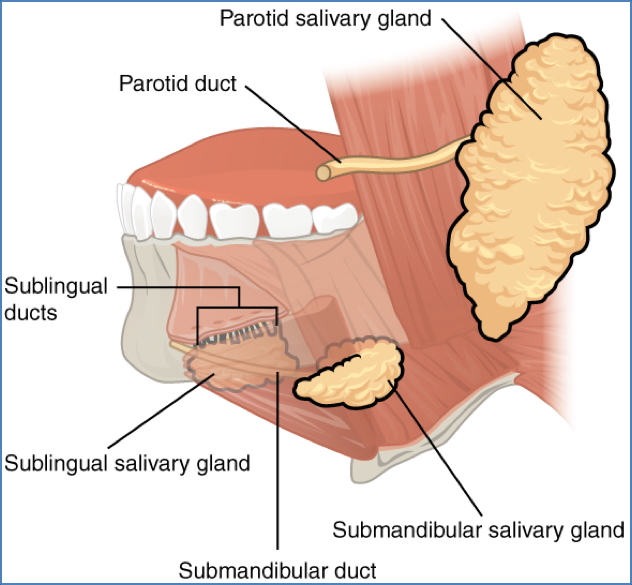
- Salivary Ducts: Parotid, submandibular, sublingual
- Arches & Passageways: Palatoglossal and palatopharyngeal arches, vestibule, oropharynx, epiglottis
- Oesophagus: Begins posterior to the epiglottis




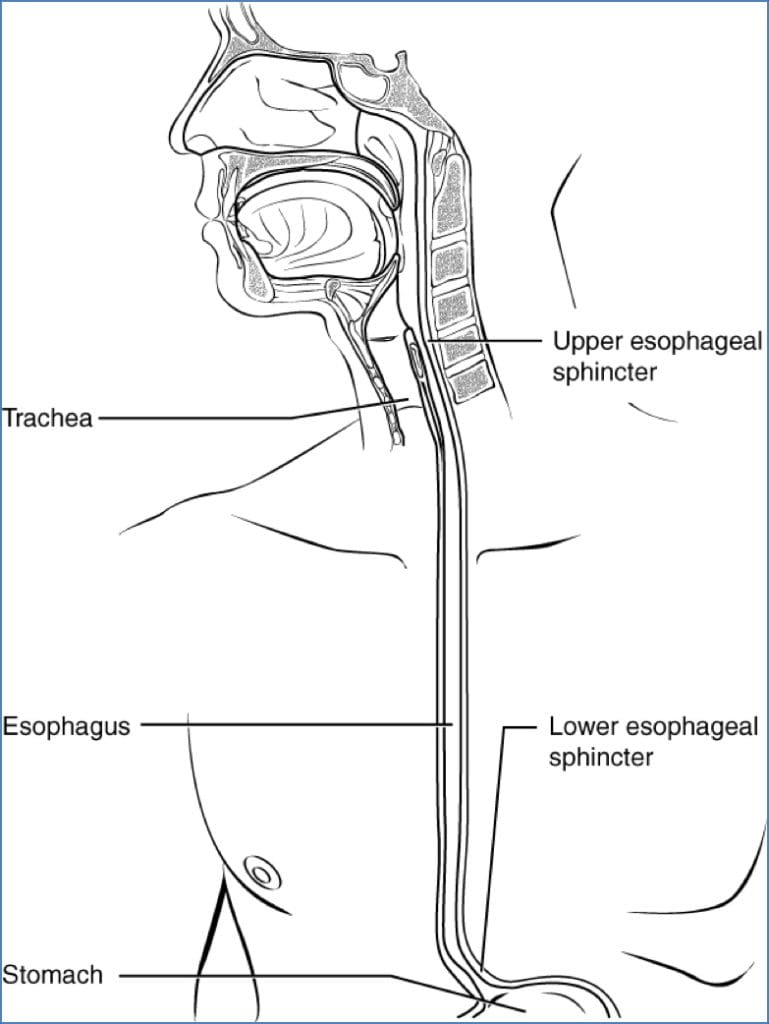
Oesophagus
Macro Anatomy
- ~25 cm long
- Passes through the diaphragm at the oesophageal hiatus
- Connects to the stomach at the cardiac orifice
- Lower Oesophageal Sphincter: Prevents reflux; dysfunction leads to GORD

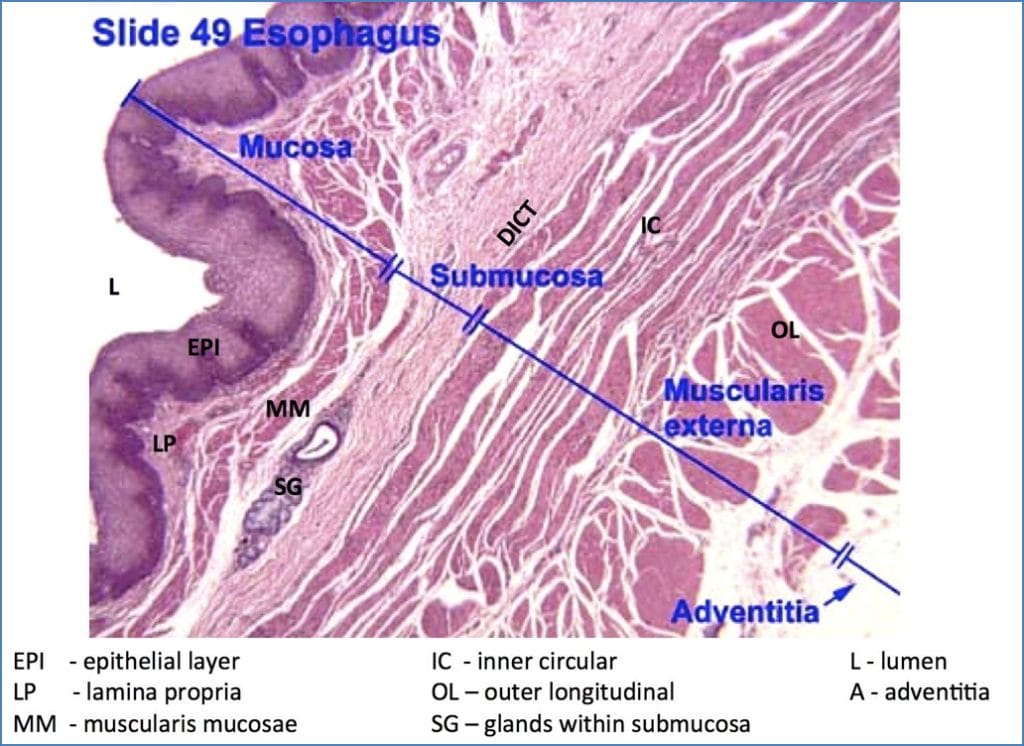
Histology
- Mucosa:
- Upper third = Stratified squamous
- Lower third = Simple columnar
- Z-line: Transition zone
- Submucosa: Dense connective tissue
- Muscularis externa: Two smooth muscle layers (for peristalsis)
- Adventitia: Outer connective tissue layer

Stomach
Functions
- Temporary storage
- Mechanical churning
- Chemical digestion (HCl, enzymes)
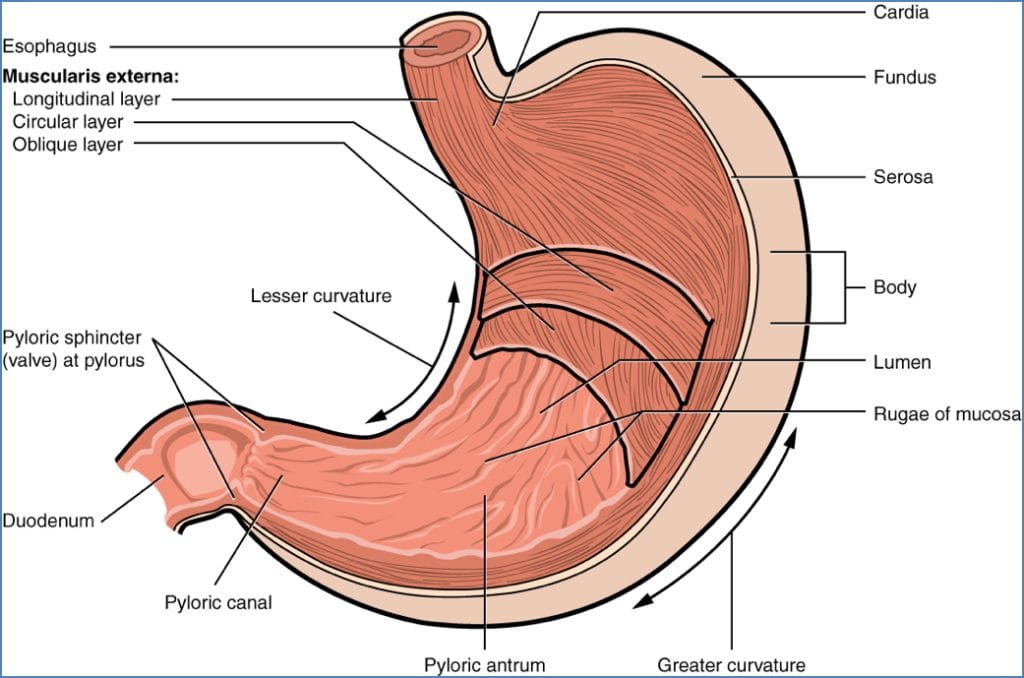
Anatomy
- Cardia, fundus, body
- Lesser & greater curvatures
- Pylorus (antrum, canal, sphincter)
- Rugae (gastric folds)

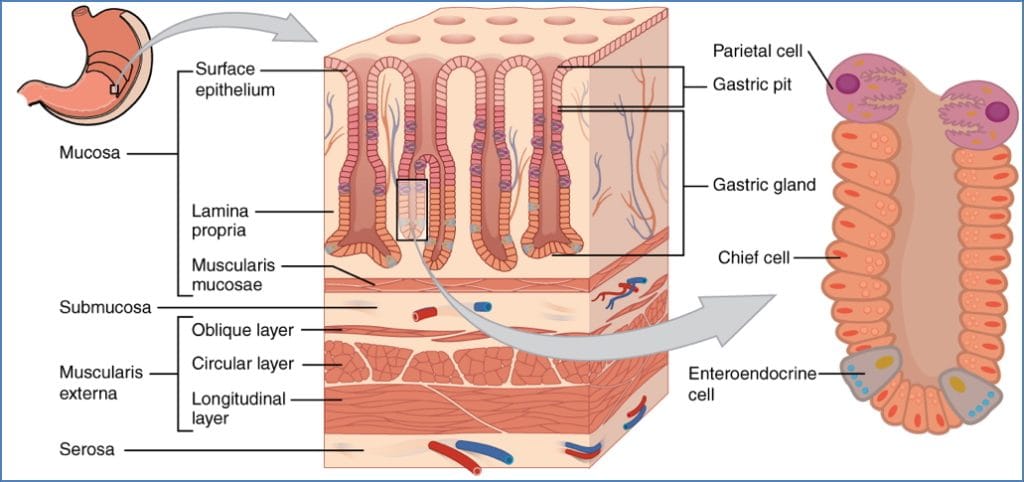
Histology
- Gastric Pits:
- Goblet Cells: Mucus
- Parietal Cells: HCl + intrinsic factor
- Chief Cells: Pepsinogen
- G-Cells: Gastrin
- D-Cells: Somatostatin

Motility
- 3 peristaltic waves/min
- Strongest at pylorus → 3 mL chyme per wave enters duodenum
Gastric Emptying
- Controlled by duodenum via enterogastric reflex
- Influenced by fatty foods, alcohol, caffeine, smoking
Vomiting Reflex
- Mediated by medulla → diaphragm contracts, cardiac sphincter relaxes
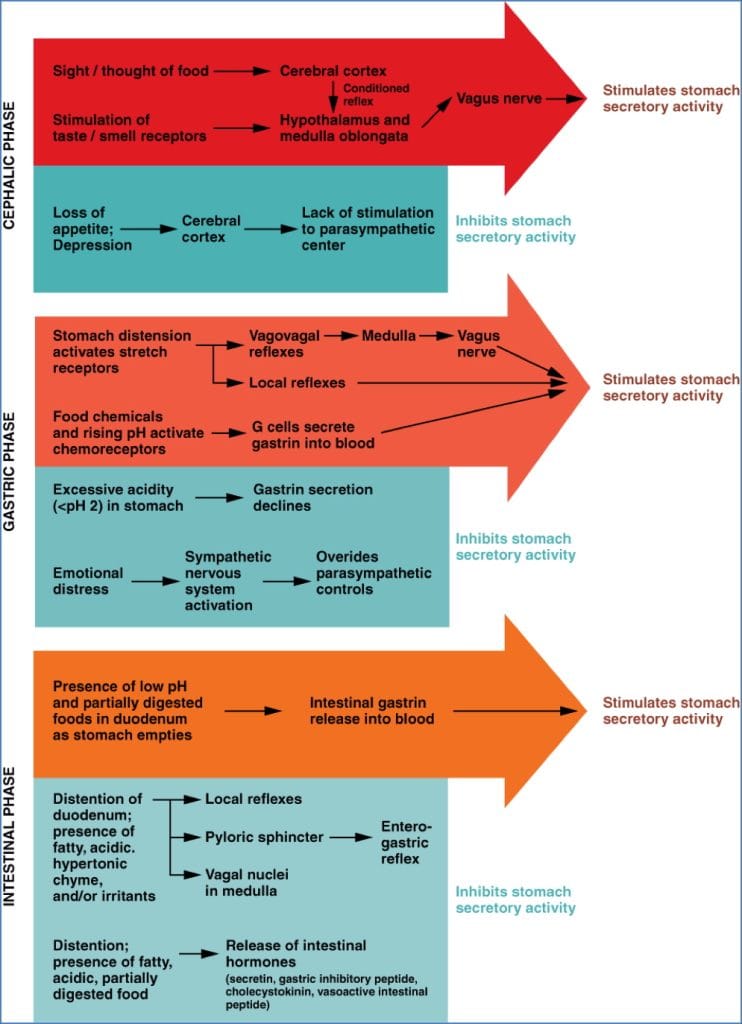
Phases of Gastric Acid Secretion
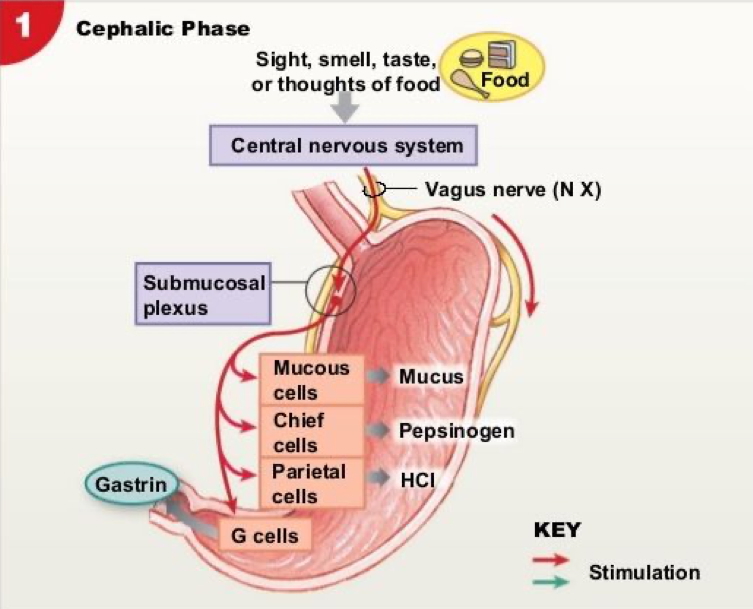
- Cephalic Phase:
- Triggered by sight/smell/thought
- Vagus nerve → G cells → Gastrin → Parietal cell activation
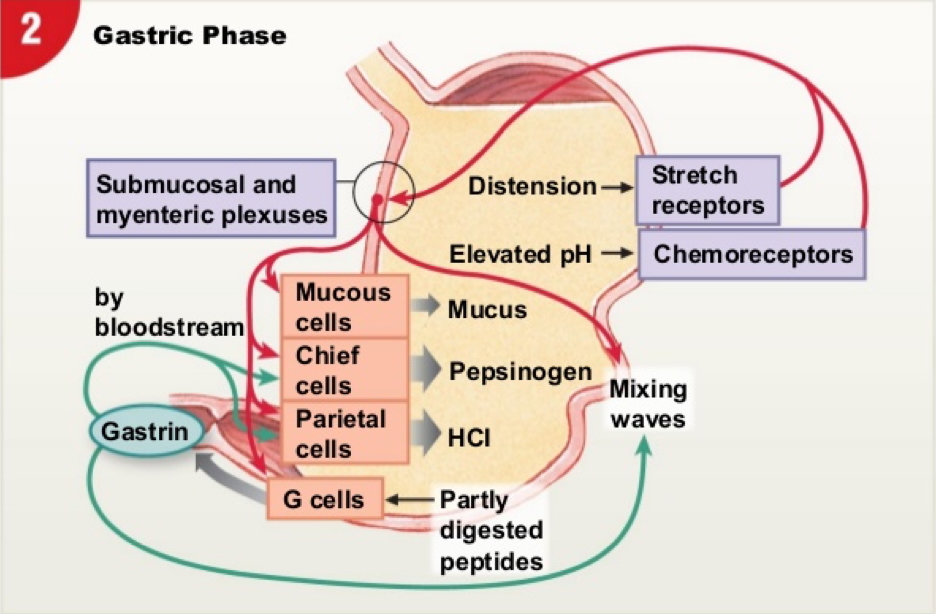
- Gastric Phase:
- Triggered by stomach distension & peptides
- Gastrin, ACh, and histamine enhance acid secretion
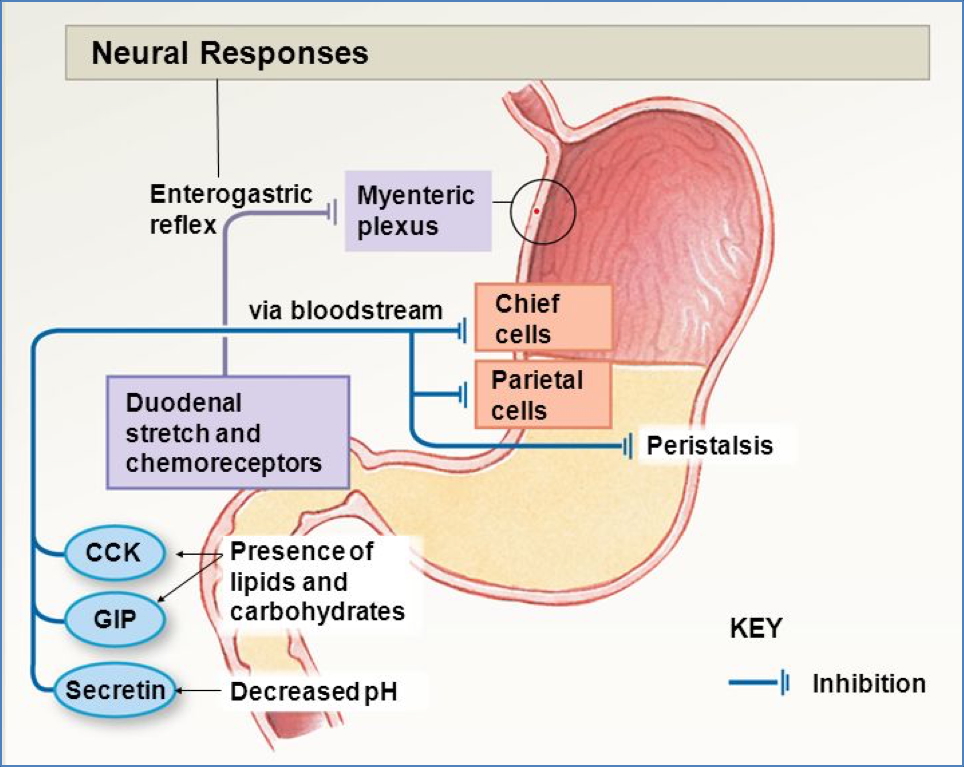
- Intestinal Phase:
- Begins with chyme in duodenum
- Initially stimulatory → then inhibitory (via secretin, CCK, VIP)




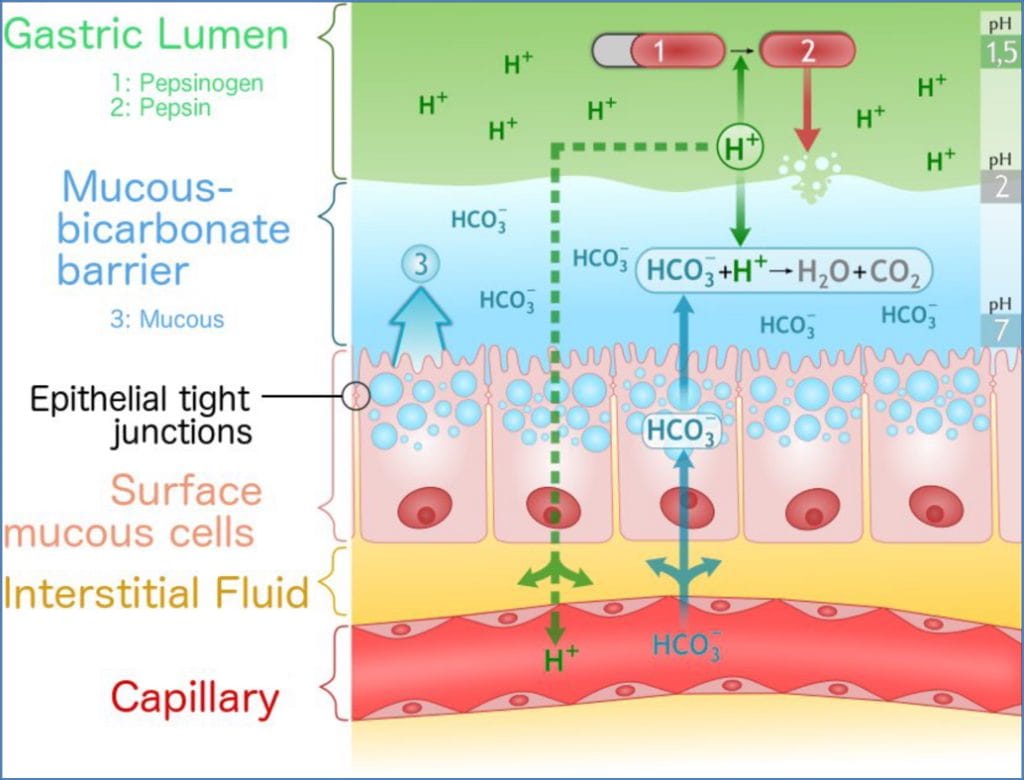
Luminal Protection & pH Regulation
- pH Zones:
- Mouth: 6.4–7.3
- Stomach: 1.5–4
- Duodenum–Rectum: 7–8
- Defence Mechanisms:
- Mucus layer
- Tight junctions
- Rapid epithelial turnover
- Alkaline secretions from Brunner’s glands, bile, pancreas

Duodenum
Anatomy
- C-shaped; connects stomach to jejunum
- Contains major duodenal papilla (entry point for bile & pancreatic juice)
Histology
- Microvilli + Goblet cells
- Brunner’s Glands: Alkaline mucus
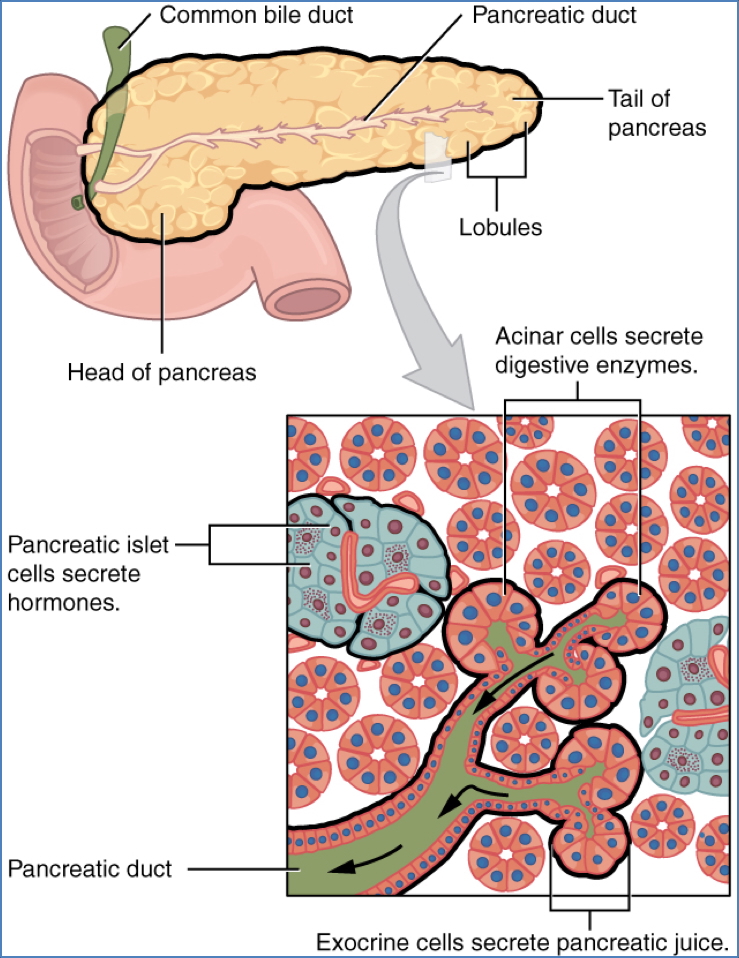
Surrounding Organs
- Gallbladder, liver, pancreas (via ducts)


Small Intestine
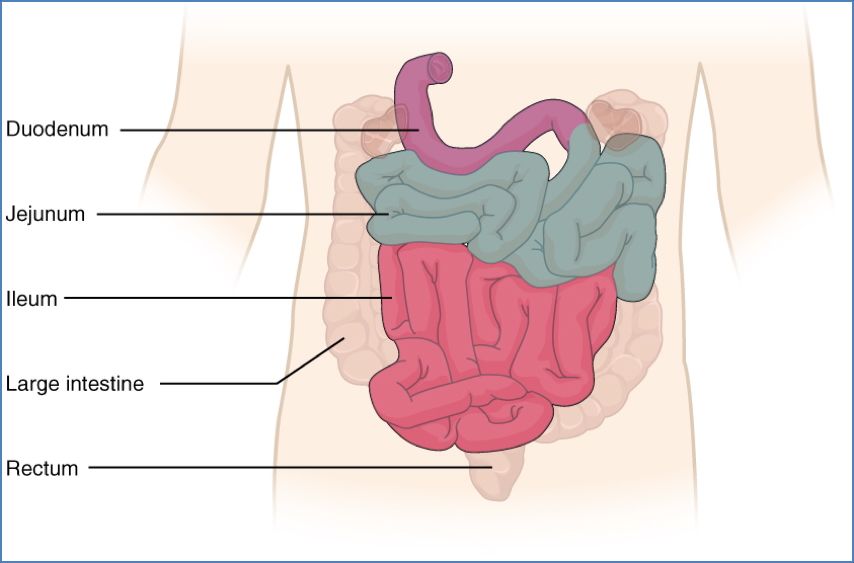
Macro Features
- Jejunum: High SA for nutrient absorption
- Ileum: Lower SA; water and electrolyte absorption
- Ends at ileocecal valve

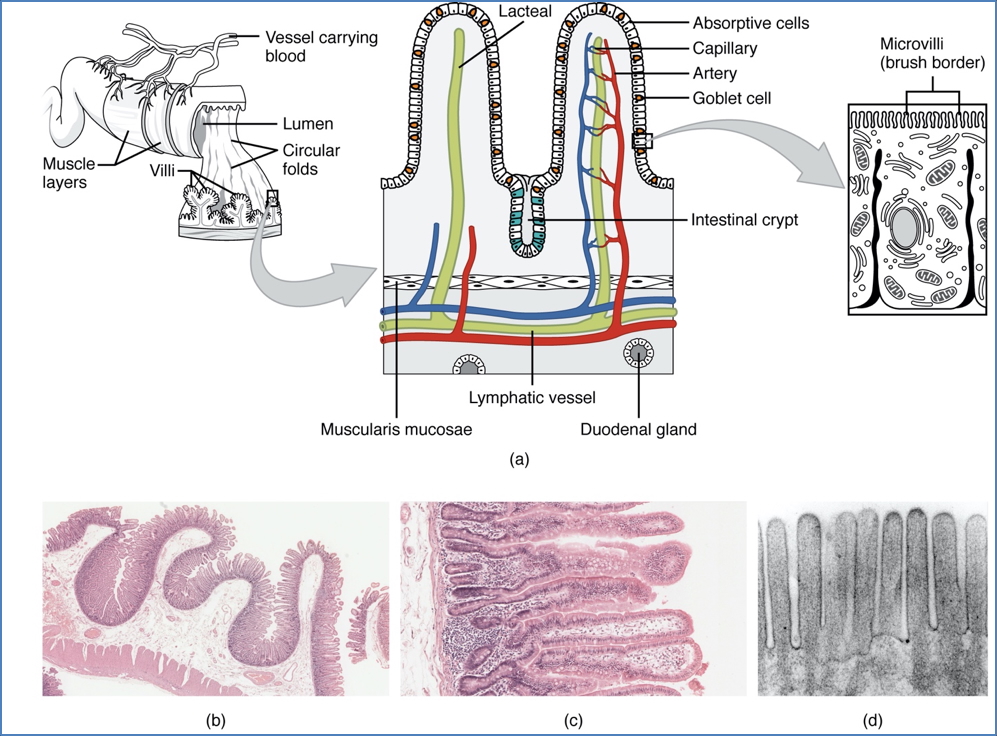
Micro Features
- Villi, microvilli, crypts of Lieberkühn
- Simple columnar epithelium, goblet cells, stem cells


Motility
- Migrating Motor Complex:
- Originates in duodenum
- Pacemaker-driven waves every ~2 hours
- Clears residual debris
Large Intestine
Functions
- Reabsorbs water
- Stores and compacts waste
Key Structures
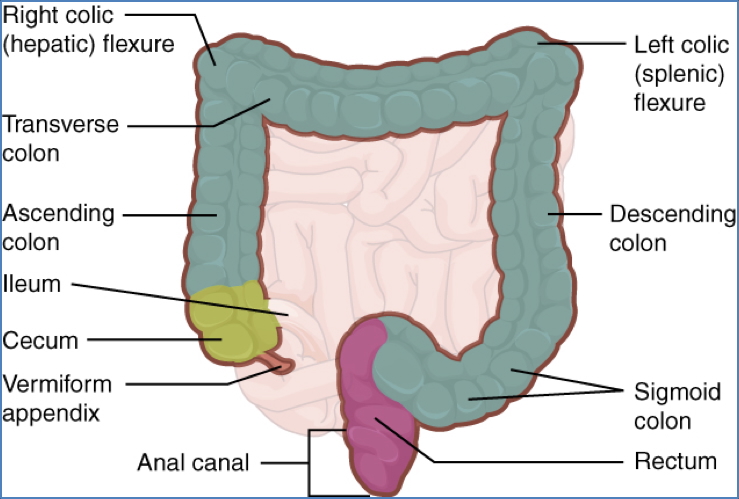
- Cecum → Ascending Colon → Right Colic Flexure
- Transverse Colon → Left Colic Flexure → Descending → Sigmoid → Rectum → Anal Canal

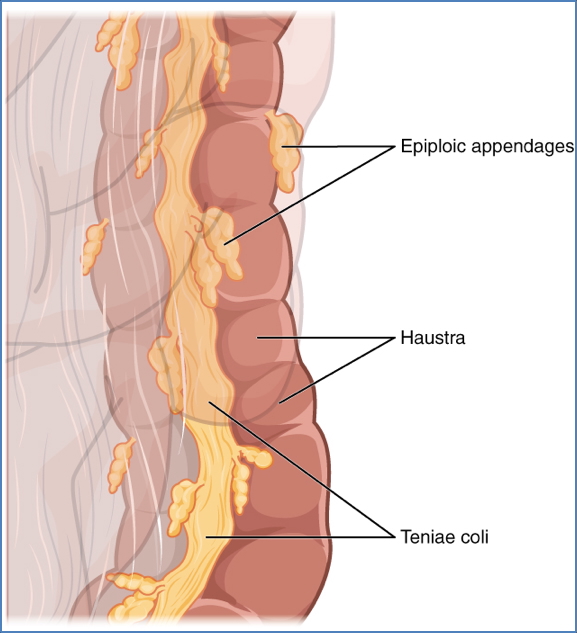
Unique Features
- Teniae Coli: Longitudinal muscle ribbons
- Haustra: Sacculations
- Epiploic Appendages: Fatty tags

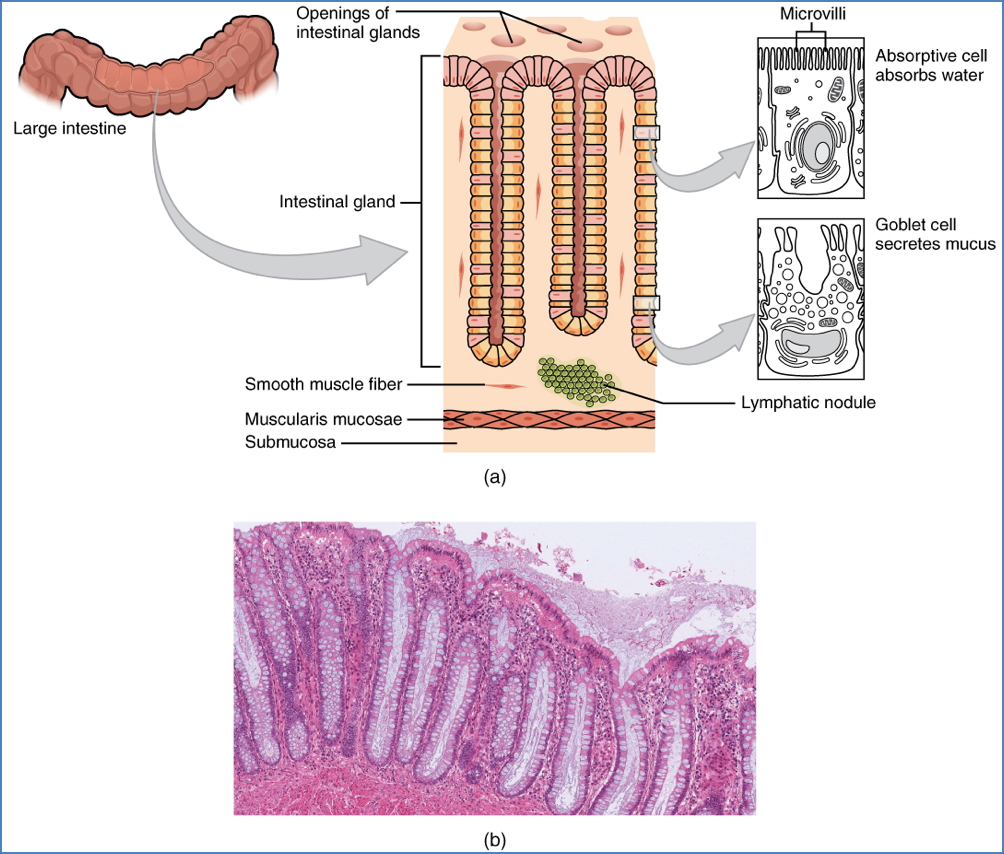
Histology
- Simple columnar epithelium + goblet cells

Motility
- Inactive most of the time
- Mass Movements: 2–3/day to move faeces to rectum
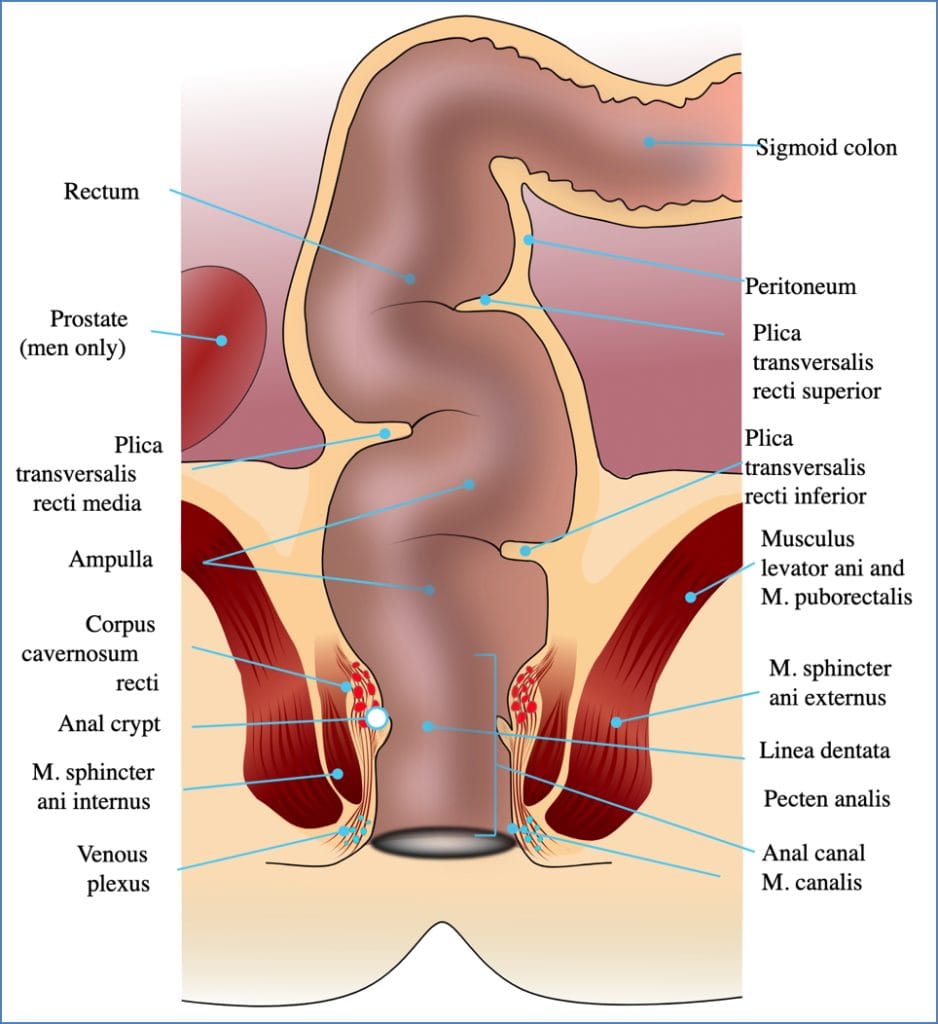
Rectum & Anus
Structures
- Rectum, Anal Canal
- Internal Anal Sphincter: Involuntary
- External Anal Sphincter: Voluntary
- Levator Ani Muscle
Motility – Defecation Reflex
- Stretch receptors → spinal reflex
- Internal sphincter relaxes
- Conscious control via external sphincter

Summary – GI Tract Anatomy
The GI tract anatomy includes highly specialised structures that optimise each stage of digestion and waste elimination. From the stratified epithelium of the oesophagus to the nutrient-absorbing villi of the small intestine and the water-absorbing features of the colon, this system is functionally and anatomically adapted end-to-end. For a broader context, see our Gastrointestinal Overview page.