Table of Contents
Overview
Lichen planus is a chronic inflammatory skin disorder characterised by itchy, purple, polygonal papules, often affecting the wrists, ankles, and mucous membranes. It is thought to be a hypersensitivity reaction, sometimes triggered by infections like hepatitis C, medications, or psychological stress. Though often self-limiting, its chronicity and mucosal involvement can impact quality of life. This page outlines its morphology, clinical subtypes, and key features.
Aetiology
- Likely multifactorial:
- Genetic predisposition
- Physical or emotional stress
- Localised skin insult (e.g. herpes zoster)
- Systemic viral infections, particularly Hepatitis C
- Contact allergens
- Drug-induced (see “lichenoid drug eruption”)
Pathogenesis
- Chronic T-cell mediated hypersensitivity reaction
- Similar underlying mechanisms to erythema multiforme, but more prolonged
- Directed against basal keratinocytes → apoptosis and inflammation
Morphology
Gross Appearance
- The “6 Ps” of lichen planus:
- Pruritic
- Purple
- Polygonal
- Planar
- Papules
- Plaques
- Lesions may be:
- Shiny, flat-topped
- Grouped or confluent
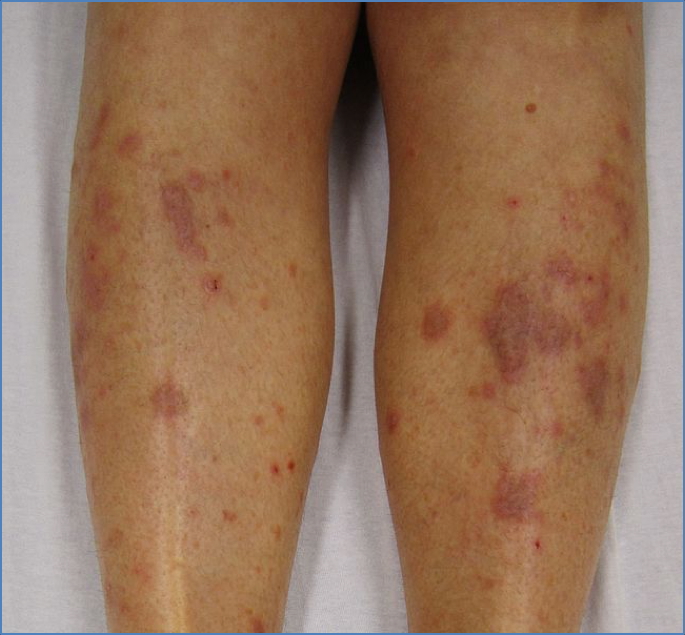

Histology
- Hyperkeratosis (scaling)
- Hyperplasia of the epidermis
- Civatte bodies (anucleate necrotic keratinocytes in basal layer)
- Band-like lymphocytic infiltrate at the dermoepidermal junction
Clinical Features
- Intensely itchy, violaceous papules and plaques
- Commonly on wrists, ankles, and lower back
- Mucosal involvement:
- Oral lesions may present as lacy white lines (Wickham’s striae)
- Genital lesions can resemble erosive or plaque-like dermatoses
- Nail involvement:
- Thinning, ridging, and even permanent nail loss
- Self-limiting in many cases:
- Resolution within 1–2 years in cutaneous disease
Subtypes
- Cutaneous lichen planus – classic skin lesions
- Mucosal lichen planus – oral/genital mucosa
- Lichen planopilaris – scalp and hair follicles → alopecia
- Lichen planus of the nails – dystrophy or loss
- Lichen planus pigmentosus – hyperpigmented macules
- Lichenoid drug eruption – drug-induced mimic of LP
Management (not in original but inferred)
- Topical corticosteroids are first-line
- Antihistamines for symptomatic relief
- Consider systemic corticosteroids, phototherapy, or immunosuppressants for severe/refractory cases
- Rule out triggering medications or underlying hepatitis C
Summary
Lichen planus is a chronic dermatosis involving pruritic, polygonal, purple papules that can affect the skin, mucosa, scalp, and nails. It often resolves spontaneously, but some variants require active treatment. Recognition of its classic morphology and subtypes is key to diagnosis and management. For a broader context, see our Skin & Dermatology Overview page.