Table of Contents
Overview – Fungal Skin Infections
Fungal infections of the skin, hair, and nails are common superficial infections, particularly in tropical and humid climates. The two major types are dermatophyte infections (tinea) and yeast infections, such as pityriasis versicolor. These conditions are caused by fungi that feed on keratin and are usually limited to the outermost layers of the skin. Although generally not serious, they are important to recognise and treat early to prevent spread, discomfort, and long-term cosmetic concerns.
Definition
Fungal skin infections are superficial mycoses that affect keratinised tissue, including the stratum corneum, hair shafts, and nails. The two primary categories are:
- Dermatophyte infections (commonly referred to as tinea or ringworm)
- Yeast infections (notably pityriasis versicolor)
Aetiology
Dermatophyte Infections
- Caused by fungi in the Trichophyton or Microsporum genera
- Transmitted via contact with infected people, animals, or surfaces
- Often affect people in humid environments or with close-contact lifestyles
Pityriasis Versicolor
- Caused by Malassezia yeast (commensal flora of skin)
- Triggered by heat, sweat, and oily skin
Pathophysiology
- Dermatophytes digest keratin → infection confined to stratum corneum
- May penetrate hair shafts, leading to hair loss
- Yeast in pityriasis versicolor overgrows and releases metabolites → suppress melanocyte function → depigmentation
Clinical Features
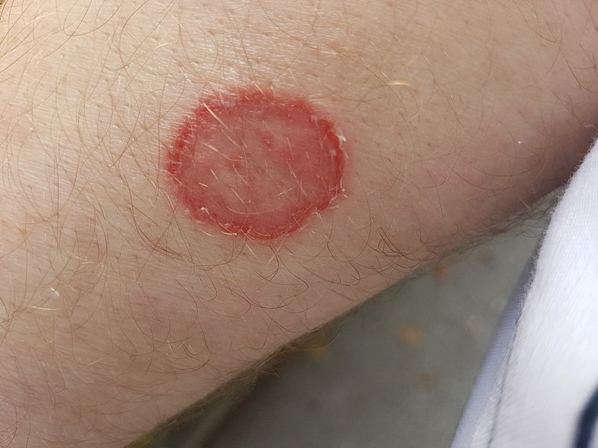
Dermatophyte (Tinea)
- Annular erythematous plaques with central clearing and peripheral scale
- Common sites:
- Tinea corporis – body
- Tinea capitis – scalp
- Tinea cruris – groin
- Non-pruritic or mildly itchy
- May present with pityriasis (skin flaking), hair loss, or thickened nails

Pityriasis Versicolor
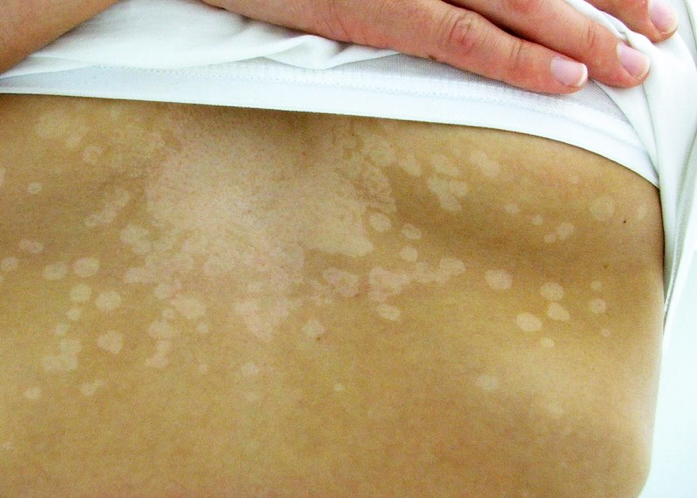
- Trunk, shoulders, neck, arms
- Well-demarcated pale, pink, or brown macules
- Fine scale
- Common in young adults
- Often more visible after sun exposure due to hypopigmentation

Investigations
- Clinical diagnosis in most cases
- Woods lamp: Microsporum canis fluoresces green
- Skin/nail/hair scrapings for microscopy (KOH prep)
- Culture if diagnosis is uncertain or patient is unresponsive to therapy
Management
Dermatophyte (Tinea)
- Topical antifungals for mild/localised disease:
- Clotrimazole
- Miconazole
- Terbinafine
- Oral antifungals for scalp, nail or extensive disease:
- Fluconazole
- Itraconazole
- Griseofulvin
Pityriasis Versicolor
- Topical treatments:
- Ketoconazole cream/shampoo
- Selenium sulphide
- Terbinafine gel
- Oral options (if topical fails or widespread):
- Fluconazole
- Itraconazole
Complications
- Recurrence is common, especially in pityriasis versicolor
- Spread to other areas or people if untreated
- Nail disfigurement in tinea unguium
- Hair loss or scarring in tinea capitis
- Psychosocial distress due to cosmetic appearance
Differential Diagnosis
- Vitiligo – depigmentation without scaling
- Psoriasis – plaques with silvery scale, not annular
- Seborrheic dermatitis – greasy scale in sebaceous areas
- Contact dermatitis – itchy, often ill-defined lesions
- Eczema – often itchy, may appear similar in distribution
Summary – Fungal Skin Infections
Fungal skin infections such as tinea and pityriasis versicolor are common superficial mycoses affecting keratinised tissues. Tinea presents as annular plaques with central clearing, while pityriasis versicolor causes hypopigmented or hyperpigmented macules. Diagnosis is often clinical but may be confirmed with microscopy or Woods lamp. Treatment includes topical or systemic antifungals depending on the severity and location. For a broader context, see our Skin & Dermatology Overview page.