Table of Contents
Overview – Intestinal Tuberculosis
Intestinal tuberculosis is an extrapulmonary manifestation of Mycobacterium tuberculosis infection, commonly seen in immunocompromised individuals or in regions with high TB prevalence. It often presents insidiously with constitutional symptoms and right iliac fossa pain due to ileocecal involvement. Understanding its pathogenesis, diagnostic criteria, and management is crucial for recognising and treating this potentially serious but curable form of extrapulmonary tuberculosis.
Definition
Intestinal tuberculosis is a granulomatous infection of the gastrointestinal tract, typically caused by reactivation or spread of Mycobacterium tuberculosis from a pulmonary focus, affecting the ileocecal region most commonly.
Aetiology
- Caused by reactivation of Mycobacterium tuberculosis
- Often secondary to pulmonary TB
- More common in immunocompromised individuals:
- HIV
- Immunosuppressive drugs
Pathophysiology
- Routes of Spread:
- Haematogenous spread from a primary pulmonary lesion
- Ingestion of infected sputum in active pulmonary TB
- Direct extension from adjacent infected organs
- Lymphatic spread from infected mesenteric or regional lymph nodes
- Site most commonly affected:
- Ileocecal region → rich lymphoid tissue and slowed transit time
- Histopathological changes:
- Granuloma formation
- Caseating necrosis
- Fibrosis and stricturing of bowel wall
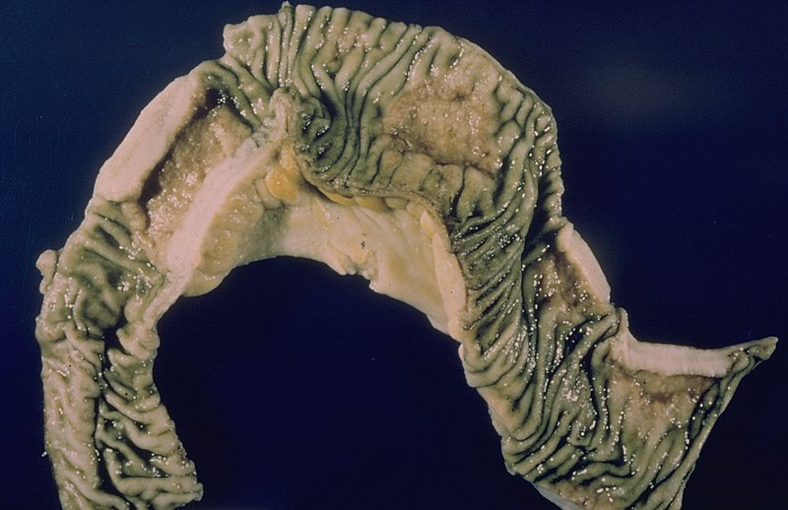
Morphology
- Macroscopic findings:
- Bowel wall thickening
- Mesenteric inflammation
- Enlarged lymph nodes
- Ulceration (especially in the transverse colon)
- Fibrotic strictures, leading to obstruction
- Microscopic findings:
- Granulomatous inflammation in lymph nodes and ulcer bases
- Central caseation surrounded by lymphocytes and giant cells

Clinical Features
- Constitutional symptoms:
- Fever, night sweats, weight loss
- Gastrointestinal symptoms:
- Right iliac fossa abdominal pain
- Palpable mass (often in the ileocecal area)
- Obstruction symptoms due to strictures
- Generalised peritonitis (if perforation occurs)
- Anaemia (chronic inflammation or blood loss)
Investigations
- Histology and culture from biopsied bowel or lymph nodes is diagnostic
- Chest X-ray:
- 50% show evidence of active or healed pulmonary TB
- Consider colonoscopy or CT abdomen for structural assessment and biopsy
Management
- Standard anti-tuberculosis therapy (typically 6–9 months):
- Rifampicin
- Isoniazid
- Pyrazinamide
- Ethambutol
- Surgical intervention may be needed for:
- Intestinal obstruction
- Perforation
- Abscesses or diagnostic uncertainty
Complications
- Intestinal obstruction
- Perforation → peritonitis
- Strictures and adhesions
- Chronic malabsorption
- Fistula formation
Differential Diagnosis
- Crohn’s disease
- Intestinal lymphoma
- Carcinoma (especially in elderly)
- Amoebiasis
- Typhoid enteritis
- Irritable bowel syndrome (in early or atypical cases)
Summary – Intestinal Tuberculosis
Intestinal tuberculosis is an extrapulmonary form of Mycobacterium tuberculosis infection, often involving the ileocecal region and presenting with fever, weight loss, and abdominal pain. It results from reactivation or spread from pulmonary TB and can cause strictures, ulceration, and obstruction. Diagnosis is confirmed through histology and culture, with treatment consisting of standard anti-tuberculous therapy. For broader context, see our Microbiology & Public Health Overview page.