Table of Contents
Overview – Breastfeeding
Breastfeeding is the optimal source of infant nutrition, offering significant benefits to both baby and mother. Breastmilk is uniquely tailored to a newborn’s changing nutritional needs and offers protective immunological benefits, including reducing the risk of infections and sudden infant death syndrome (SIDS). Clinicians must be equipped to support breastfeeding, recognize common challenges, and provide evidence-based guidance for overcoming issues such as undersupply, reflux, or mastitis. Effective counselling around breastfeeding plays a crucial role in early child development and maternal health.
Benefits of Breastfeeding
For the Baby
- Nutritionally complete — adapts to the baby’s needs
- First half of feed = hydrating and sugary; second half = rich in fats
- Protects against infections and reduces risk of SIDS
- Promotes development of:
- Eyesight
- Speech
- Jaw and oral structures
- Supports early flavour exposure (via maternal diet) → better acceptance of solids
For the Mother
- Promotes bonding via skin-to-skin and oxytocin release
- Free, hygienic, and convenient (no sterilising or preparation needed)
Guidelines for Feeding
- Feed every 2–3 hours for the first 3 months (>8 feeds/day)
- Each feed should last 20–30 minutes
- Signs of adequate intake:
- 5 wet disposable nappies / 24 hours
- 6–8 wet cloth nappies / 24 hours
- If baby seems persistently hungry:
- Express milk between feeds
- Supplement with pre-expressed milk or formula
Duration of Breastfeeding
- Exclusive breastfeeding recommended for at least 6 months
- WHO: Continue breastfeeding alongside solids up to 2 years or beyond
- After 12 months, continuation is based on mother-baby preference
Breastfeeding Technique
Feeding Setup
- Comfortable chair with back support
- Stay hydrated — large glass of water on hand (avoid caffeine)
- Baby held chest-to-chest; aim nipple at upper palate
- Ensure baby’s nose is clear
- Listen for regular swallowing
- Allow baby to burp post-feed
- Change nappy
- Offer second breast if still hungry


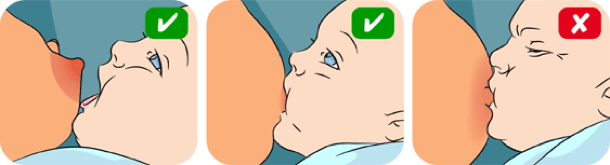
Attachment
- Hold baby nose-to-nipple, trigger rooting reflex
- Bring baby to breast chin-first
- Good attachment signs:
- Most of areola inside baby’s mouth
- Chin touches breast, nose remains clear
- Deep, rhythmic sucking with intermittent swallows
- Reattach if latch is incorrect

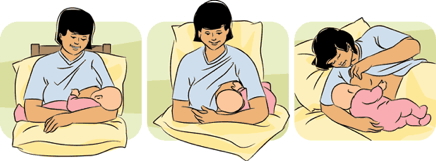
Breastfeeding Positions
- Front hold (cradle)
- Underarm hold (good for twins)
- Lying down (ideal after caesarean)
- Twin hold
- Public feeding positions



Common Breastfeeding Challenges
Sore Nipples
- Caused by poor attachment
- Solutions:
- Nipple shields (short-term)
- Hand expression or breast pump for gentler expression
Nipple Infections
- Causes: S. aureus or Candida from cracked nipples
- Treatment:
- Moisturisers between feeds
- Topical antibiotics/antifungals
Blocked Milk Ducts
- Tender breast lump without systemic illness
- Management:
- Frequent feeding (start on affected breast)
- Massage, warm compresses
- Check bra fit
- Watch for mastitis if symptoms persist >12 hours
Mastitis
- Inflamed, painful, red breast + flu-like symptoms
- Management:
- Urgent GP review → antibiotics
- Continue breastfeeding to avoid abscess
Engorgement / Oversupply
- Baby may struggle with fast flow or develop wind
- Management:
- Feed from one breast per session
- Express briefly before feeding
- Ice-pack or cabbage leaf post-feed
Undersupply
- Signs:
- <5 wet disposables or <6–8 cloth nappies/day
- <1 bowel motion/day (if <6–8 weeks old)
- Poor weight gain or weight loss
- Management:
- Supplement with expressed milk or formula
- Frequent breastfeeding or pumping
- ‘Top-up’ feeds 20–30 mins post-feed
Reflux
- Common in first 6 months; typically benign
- Signs: large-volume spit-ups
- Management:
- Feed in upright position
- Elevate cot head
- If failure to thrive or pain → refer to paediatrics
Breast Refusal
- Causes: illness, discomfort, poor attachment, overstimulation
- Management:
- Try different positions
- Offer when baby is sleepy
- Express into mouth
- Use quiet environment, soft music
Bottle Feeding
If breastfeeding isn’t possible:
- Use expressed breast milk in a bottle
- Use properly prepared infant formula (only safe alternative)
Summary – Breastfeeding
Breastfeeding offers unmatched benefits for both infant and maternal health and is recommended exclusively for the first 6 months of life. From nutritional advantages to immune protection and bonding, it sets the foundation for lifelong wellbeing. Understanding breastfeeding technique, recognizing challenges like mastitis or oversupply, and supporting parents through these early months are vital skills. For a broader context, see our Reproductive Health Overview page.