Table of Contents
Overview – Hemolytic Uremic Syndrome
Hemolytic uremic syndrome (HUS) is a serious thrombotic microangiopathy that primarily affects the kidneys. It is most commonly seen in young children following gastrointestinal infection with Shiga toxin-producing Escherichia coli (STEC), especially serotype O157:H7. HUS is characterised by a clinical triad of microangiopathic hemolytic anaemia (MAHA), thrombocytopenia, and acute kidney injury. Prompt recognition is crucial, as complications can include multi-organ failure and neurological deficits.
Definition
- Hemolytic uremic syndrome (HUS) is an acute condition marked by:
- Microangiopathic hemolytic anaemia
- Thrombocytopenia
- Acute renal failure
- Often follows shiga-toxin–producing E. coli (STEC) infection
Aetiology
- Most common cause:
- Shiga-toxigenic Escherichia coli (STEC), also known as enterohemorrhagic E. coli (EHEC)
- Other triggers:
- Shigella dysenteriae type 1 (less common)
- Rare: complement-mediated or familial HUS variants
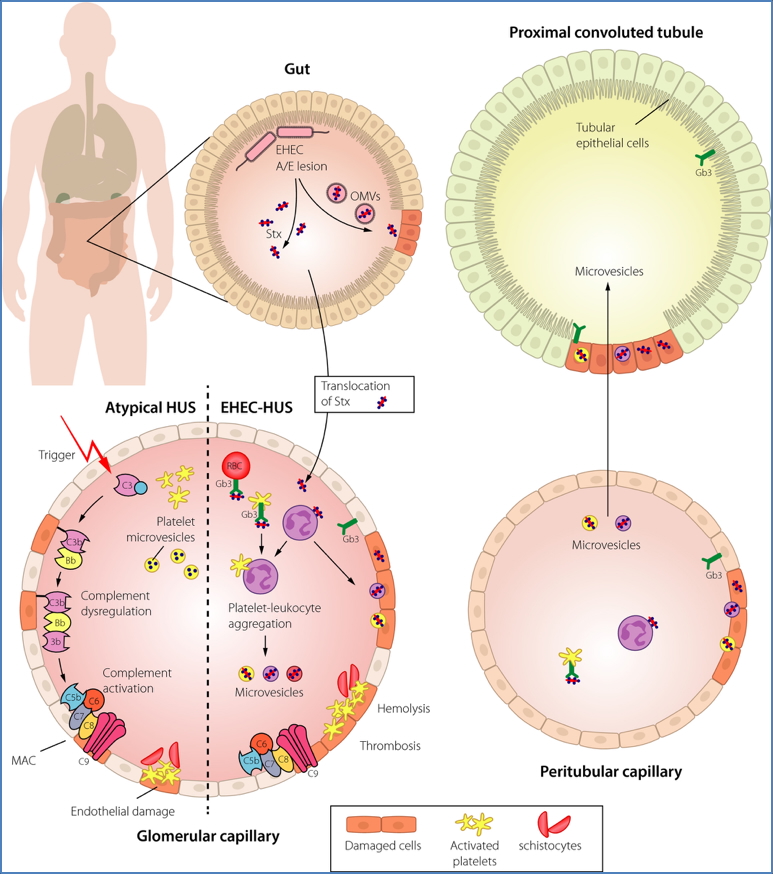
Pathophysiology
- E. coli adheres to the intestinal wall and releases Shiga-like toxin
- Toxin enters the bloodstream → binds to leukocytes
- WBCs deliver the toxin to glomerular endothelial cells →
- Endothelial injury
- Platelet activation and widespread microthrombi
- Leads to:
- Mechanical hemolysis (schistocytes)
- Reduced renal perfusion → acute kidney injury
- Elevated serum urea and creatinine

Clinical Features
- Most common in children under 5 years, and elderly adults over 75
- Gastrointestinal prodrome:
- Bloody diarrhoea (post-EHEC infection)
- Systemic features:
- Weakness, fatigue, jaundice (due to haemolysis)
- Oedema and oliguria (from AKI)
- Fever
- Neurological complications:
- Visual disturbances
- Confusion or altered mental status
- Seizures, stroke, or coma in severe cases
Investigations
- Blood tests:
- Thrombocytopenia
- Anaemia with schistocytes on blood film
- Elevated lactate dehydrogenase (LDH)
- Raised urea and creatinine
- Urinalysis:
- Proteinuria
- Haematuria
- Specific tests:
- Positive Shiga toxin PCR (stool)
- Exclude other causes of thrombotic microangiopathy
Management
- Supportive care is key:
- Fluid and electrolyte balance
- Monitor renal function and urine output
- Dialysis if required
- Avoid antibiotics and anti-motility agents:
- Bacterial lysis may release more Shiga toxin
- Plasma exchange or eculizumab (for atypical HUS, not typical STEC-HUS)
Complications
- Acute renal failure
- Chronic kidney disease or ESRF
- Neurological sequelae (stroke, seizures)
- Mortality in severe untreated cases
Differential Diagnosis
- Thrombotic thrombocytopenic purpura (TTP)
- Atypical HUS (complement-mediated)
- Sepsis with DIC
- Lupus nephritis
- IgA vasculitis (Henoch–Schönlein purpura)
Summary – Hemolytic Uremic Syndrome
Hemolytic uremic syndrome (HUS) is a life-threatening complication of Shiga toxin-producing E. coli infection, especially in children. It presents with hemolytic anaemia, thrombocytopenia, and acute kidney injury. Management is mainly supportive, and antibiotics are avoided due to toxin release risk. For a broader context, see our Renal Overview page.